Neck Injuries: The 9 Most Common Types
Neck injuries, aka cervical spine injuries, vary in severity and type. An injury to your neck may be preceded by accident, trauma to the area, falls, degenerative changes that take place in the spine or a combination.
Here's an overview of the most common types plus information on their symptoms, treatment, and more.
Neck Injuries Affecting Soft Tissue
Damage to one anatomical part in your neck often means damage to others. This is because the parts of your neck are connected. Bones, joints, soft tissue, and nerves in the cervical spine all work together to hold up and move your head. As an example, whiplash may result in one or several diagnoses, including muscle strain, ligament sprain, and/or disc injury.
The good news is that most of the time, neck injuries mainly affect soft tissue — your muscles, tendons, ligaments, and/or fascia. But every type of cervical spine injury, including those that involve the bones, joints, and discs, will also affect your muscles at least to some extent.
The first three injuries on the list are ones that affect the soft tissue.
Neck Injuries That May Affect Nerves and/or the Spinal Cord
Some neck injuries affect or damage the nervous system, and these can get pretty serious. Nerve involvement generally occurs when one or more spinal structure comes into contact or puts pressure on either a spinal nerve root, the spinal cord, or both.
The remaining injury descriptions in this article talk about those that in some way, whether mild or serious, affect some aspect of the nervous system.
Crick in the Neck

Have you ever awakened with a nasty neck crick and wondered what it could be?
Unfortunately, crick in the neck is not a medical diagnosis. Usually, muscle spasm, trigger points, arthritis, and/or a disc problem underlie the pain.
Neck cricks tend to be brought about by simple things such as sleeping with your neck in an awkward position, spending long hours at the computer, and/or sudden movements of your cervical spine.
What should you do for a neck crick? Most of the time, at-home therapies such as aspirin or Tylenol, also known as acetaminophen, reduced activity, and gentle movement are all it takes to relieve the pain. Waiting it out plays a big role, as well.
If you find that the pain of your crick lingers for longer than a week, or it disrupts your usual activities, it's likely time to see your doctor. The same is true if you've been diagnosed with a neck problem in the past or you have (or have had) a serious health condition such as cancer.
Muscle Strain

Elizabeth Young/Getty Images
A neck strain is an injury to the muscles that attach to and move the head and upper part of the spine. Symptoms include muscle spasm, reduced flexibility, and pain.
Strains are graded, meaning that they range from mild to severe.
Grade I strains are mild and are often treated by modifying activity to a level where the pain is tolerated, without giving into complete bed rest. Also, taking an over-the-counter pain medication is a common way to get past the pain of a mild strain. As with a neck crick, if the pain lasts longer than a week, or if it disrupts your usual activities, see your doctor.
With a Grade II neck strain, the injury is limited to the muscle only. Like a Grade 1 strain, your neck pain is likely not indicative of other types of structural damage.
But when it comes to Grades III and IV, it is. According to the Quebec Task Force on Whiplash-Associated Disorders, Grade III neck strain is associated with nerve damage. In this case, you may, among other things, get weak and/or feel electrical sensations down one arm. With these injuries, making an appointment with your doctor as soon as possible will likely give you the best chance of a full recovery.
Needless to say, Grade IV neck strains are the most serious of all. The Quebec Task Force says these are related to fracture or vertebral dislocation. This injury requires immediate medical attention.
Neck Sprain

Sprains are injuries to ligaments. (Ligaments are strong bands of connective tissue that hold bones together.)
Neck sprains can be caused by falls or sudden twists that overload or overstretch one or more joints in your cervical spine. Another cause is repeated stress to the joint.
According to the American Academy of Orthopedic surgeons, symptoms of a neck sprain can be very varied but may include pain at the back of your neck that gets worse when you move, pain that comes on slowly and peaks after about 24 hour hours, headache at the back of the neck, muscles spasms and pain in your upper shoulder, neck stiffness, and/or numbness, weakness, or tingling in your arm.
Neck sprains can also bring on less structural type symptoms, including a sore throat, mood changes, difficulty concentrating or sleeping and more, the AAOS says.
Similar to neck strains, neck sprains can be mild, moderate, or severe and are graded. This may mean, for example, that if you have tingling down one arm, your sprain is a Grade III. Always check with your doctor to be sure.
If you suspect someone in your environment has a severe neck injury of any kind, you should immobilize their spine and call 911 immediately. Do not attempt to move them unless doing so is the only way to save their life.
For minor and moderate sprains, generally resting and icing the area is recommended, as is taking anti-inflammatory medication. Generally, an over the counter will do. Getting it checked by a doctor is important, as well.
Whiplash-Associated Disorders (WAD)
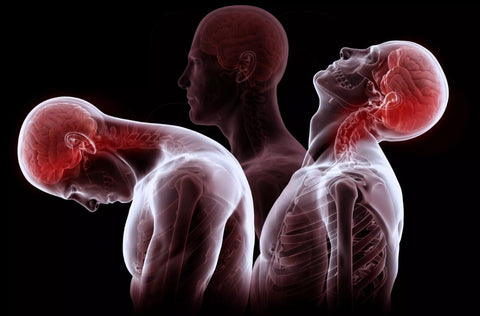
Whiplash (WAD) is a set of symptoms following a movement event in which the head is thrown first into hyperextension and then quickly forward into flexion. It's most often due to car accidents, but may be caused by sports injuries, falls, or trauma.
Like a neck crick, WAD is not a medical diagnosis. It's an episode that can lead to any number of diagnoses from strain to a herniated disc and sometimes more.
Whiplash may damage joints or discs, which in turn may irritate spinal nerve roots or, more rarely, the spinal cord, causing nerve symptoms.
Depending on the exact nature of the injury, symptoms can include pain, weakness, numbness, tingling, or other electric-type sensations that go down one arm. Stiffness, dizziness, or disturbed sleep are also possible. Note that symptoms may be delayed a day or two following the whiplash event.
Research suggests that a multi-modal approach to treating whiplash can be effective. This may include heeding your doctor's advice, getting some hands-on soft tissue work from a physical or massage therapist, medication, wearing a collar, and/or therapeutic exercise.
Herniated Disc
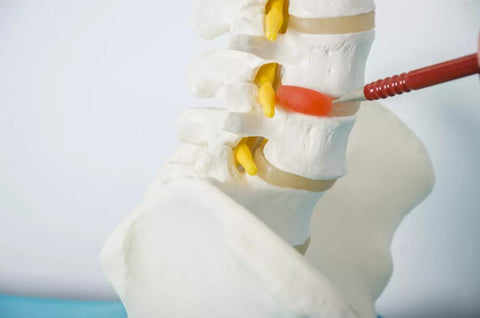
A herniated disc occurs when the soft substance that is normally contained to the inside of the disc (called the nucleus pulposus) escapes. Should this jelly-like substance land on a nerve root, which it often does, you'll likely feel pain and/or have nerve-related symptoms. Nerve-related symptoms generally includes weakness, numbness, a burning sensation, or electrical shock sensation that go down one arm.
Tears in the tough outer fibers of the disc (called annular tears) may lead to a herniation. Annular tears may be brought on by either repeated or a sudden, forceful stress to the spinal joint. Treatment generally starts with medication and physical therapy but may proceed to surgery as needed.
Herniated discs can happen anywhere along the spine where one of the shock-absorbing cushions are located, including of course, in the cervical spine, or neck, area.
Stingers and Burners

Named for the way they feel, stingers and burners are temporary injuries to the spinal nerve root or brachial plexus. They occur most often in football players, especially tacklers, as well as other contact-sport athletes.
Stingers and burners may be caused either by an abrupt tilt of the head or when the head and shoulder are forced in opposite directions at the same time.
Symptoms include burning, stinging, numbness/weakness, or an electrical sensation down one arm. You may feel a warm sensation along with the other symptoms.
If a stinger or burner is severe or lasts longer than a few minutes, see a doctor. If you are an athlete with stenosis, your risk is higher and your doctor may suggest that you retire from your sport to avoid a catastrophic neck injury.
Neck Fracture
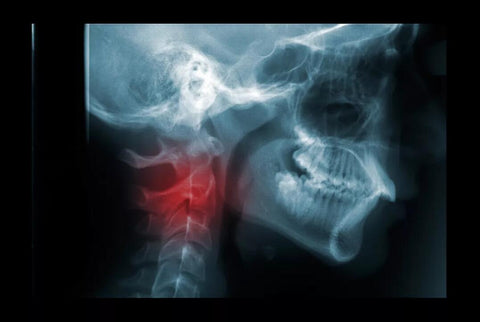
A neck fracture is a break in a cervical bone. It may be caused by trauma, a fall, or degenerative changes in the spine. The angle of force at impact often determines the type and severity of the break.
Football players who block with their head are at high risk for cervical fractures. Elderly people with osteoporosis are also at risk, because of their fragile bones. The most serious neck fractures are generally accompanied by a dislocation.
Treatment depends on a lot of things, including your age, other medical conditions, and the extent of damage to your spine. If a fracture destabilizes your neck, you may need to wear a halo brace.
Prevention is the best treatment strategy for a neck fracture. If you have osteoporosis or osteopenia, ask your doctor or physical therapist about prevention ideas.
Cervical Dislocation

Dislocation occurs when a neck bone moves out its normal position, creating spinal instability. When a neck bone is dislocated, either an injury or degenerative changes disrupt the ligaments that normally hold it in place, causing it to separate from the bone below.
When brought on by trauma, a dislocation may be accompanied by fracture.
In the most severe dislocation, the bone is fully displaced forward (called jumping), and it locks in this position. The ligaments rupture completely. Dislocations may damage the spinal cord and/or require surgery.
Less severe forms occur when the bone does not move all the way out, or when only one side fully displaces. Mild dislocations may go back in place on their own, and the soft tissue treated by wearing a collar.
Spinal Cord Injury

A spinal cord injury (SCI) occurs when a fracture, dislocation, or other neck injury damages the spinal cord. If the spinal cord is damaged at the third cervical vertebra or above, the person may die or need a respirator to stay alive.
People living with SCI often endure a lifelong disability with complete or incomplete paralysis below the level of injury.
The timeliness of emergency care and the type of first aid and medical treatment immediately given are especially critical to survival and subsequent quality of life following any serious neck injury. If someone in your environment has a traumatic incident, you should assume they have a serious or even life-threatening neck injury such as spinal cord injury, and follow Red Cross guidelines.
Here're neck braces of the most common types:
- Choosing a selection results in a full page refresh.



2 comments
GoMedii
Thank you for explaining.
Spine Surgeon In Noida
GoMedii
thanks for explaining.
Spine Surgeon In Noida